How a Dedicated RCM Team Lightens Frontliner’s Workload
On a daily basis, an average healthcare professional is loaded with core tasks such as assessing the patient, plan treatment course, execute tests and diagnostic procedures all the while documenting every step provided and performed to the patient. Simply put, their workload is never light. When administrative tasks such as coding, billing, patient concierge and claims processing add to their existing work, it may distract them from their core responsibilities.
And with the increase in workload demands and a significant decrease in healthcare workforce and resources, medical professionals need the back-up support they can get from Revenue Cycle Management (RCM). This article will showcase 3 ways a dedicated RCM team helps lighten the burden from healthcare providers.
- Correct billing and collection errors freeing healthcare providers from administrative tasks
Medical billing and collection errors account for 80% of problems for healthcare revenue management. Examples of these are;
- Upcoding: where entering the code of a more serious medical condition than what was treated inflates the bill
- leftover billing
- duplicate billing
- incorrect patient information
- mismatched diagnosis codes
These errors make it difficult to ensure collections from patients. If your primary healthcare team has to handle these administrative tasks, they would need to spend more time completing paperworks and trying to adjust to the latest changes in medical billing than actually performing care and treatment related responsibilities. But having a dedicated RCM team will help your business overcome these challenges, not only because they are trained with the latest billing and coding standards such as the ICD-10, they also focus solely on getting these tasks done right with quality and proficiency (i.e. <1hour turnaround time and zero coding errors). In return, this will lead to an increase in the level of patient care and thus make practices more patient-centric.
- Improve business revenue and practice profitability
According to the Medical Group Management Association (MGMA), 50-65% of denials go unworked. It means that healthcare businesses are missing out on revenue and on the opportunity to detect denial trends to prevent future occurrences if there is no dedicated team to perform revenue management tasks.
While this can happen at various points in the revenue cycle, denial management is a common weak spot for many practices. That is why outsourcing an RCM team that can solely perform tasks from claims submission to payer collections to a trusted partner can help you avoid revenue slipping through the cracks. As they focus on RCM cycle processes, there will be increased cash flow and more prospects for optimization. On the other hand, this promotes clarity between responsibilities from your in-house healthcare team by allowing them to devote their time and energy on patient care.
- Business recovery support allowing patient-centric efforts from healthcare team
A trusted partner who can build you a great, high-performing RCM team will be your additional support during business recovery because they help you overcome the limited supply of workforce which not only lighten your in-house healthcare team’s workload but also allows you to save 70% on operation cost, innovate care technologies to ease manual labor and process improvement for your healthcare business, and ensure patient data security with an established Information and Cybersecurity processes.
A reliable partner and RCM team mitigates disruption from major industry changes. Not only would the right partner help you manage ICD-10 updates in coding, they are more likely to generate and complete higher volume of denials at a required turnaround time and also share industry expertise to help you navigate through any industry transition more easily. Whether it’s ICD-10 or another monumental shift, outsourcing to a trusted partner can be a great way to mitigate disruption during times of change.
Building Top RCM Teams
Building the right team creates a well-oiled RCM process. In return it can result in:
- 95% coding, billing and documentation accuracy
- 1 hour turnaround time
- Improved denial management rate
- HIPAA and DPA-20212 compliant
And turning to a trusted outsourcing company to help you build this team gives you access to a world-class pool of talent all the while saving up to 70% operational cost without compromising quality of work and maintaining operational excellence. The right partner also has an established Information Security in place to ensure patient data confidentiality regardless if working on site or remotely.
Partnership with Infinit-O
Infinit-O’s mission is to create endless opportunities for your company to realize its full potential.
Infinit-O Key Benefits:
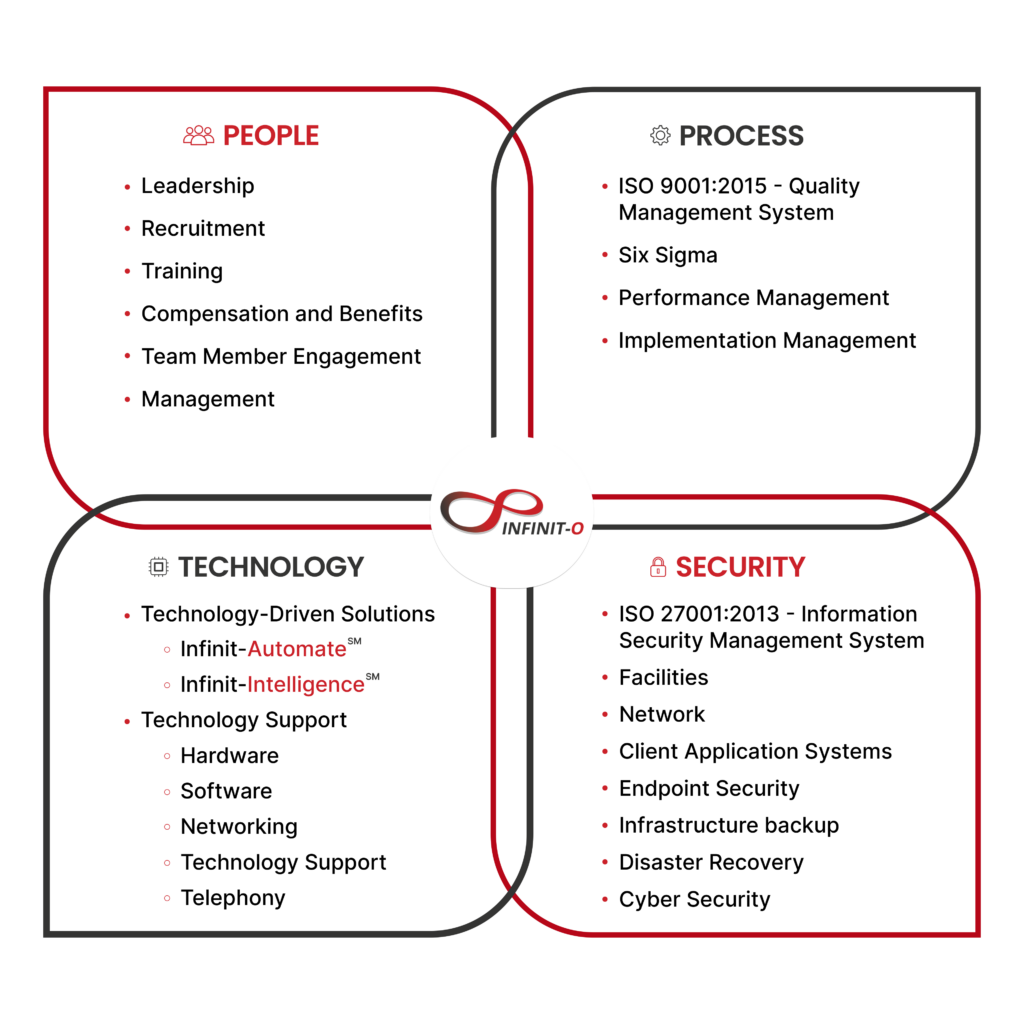
We can build you a great, high-performance Revenue Cycle Management team composed of:
Patient Support Services
- Patient Concierge Specialist
- Insurance Verification Specialist
- Collections Specialist
- A/R Specialist
Provider Management Services
- Medical Coders
- Medical Billers
- Claims Processors
- Enrollment Processors
- Denial Management Specialist
Health Analytics and Risk Management Services
- Healthcare Analyst
Others
Let’s work together to build a great RCM Team.
Infinit-O is the trusted customer-centric and sustainable leader in Business Process Optimization to Small and Medium businesses in the Financial Services, Healthcare and Technology sectors by delivering continuous improvement through technology, data and people.







This site is protected by reCAPTCHA and the Google Privacy Policy and Terms of Service apply.